While the COVID-19 crisis affects everyone, those who were already marginalized – women, ethnic minorities, and the poor – are likely to suffer the most. That is why no pandemic-response strategy is complete without a plan to ensure uninterrupted access to health care for all.
BANGKOK – Last month, Sheuly rushed into a Dhaka hospital in need of emergency treatment. The 25-year-old Bangladeshi woman had just given birth at home – thinking it a safer setting than the hospital during a pandemic. But as she began to suffer from post-partum hemorrhage – one of the leading causes of maternal death worldwide – avoiding exposure to COVID-19 was the furthest thing from her mind. The same was true of Majufa Akter, the midwife who sprang into action and saved Sheuly’s life, despite not having yet received adequate personal protective equipment (PPE).
Giving birth is an intense moment in a woman’s life under any circumstances. Doing so during a pandemic imbues the experience with a new form of stress. Mothers do not know whether to go to hospitals – where they fear exposure to the coronavirus, personnel shortages, or separation from their partners – or to give birth at home, where medical complications often become far riskier. This is just one example of how the imperative of managing the COVID-19 pandemic is complicating the delivery of essential health services – and leaving women, in particular, highly vulnerable.
Around the world, when health systems are overstretched, services for women are often among the first to suffer, resulting in increased maternal and child morbidity and mortality. To illustrate the risks, we have modeled the pandemic’s possible impact on three key sexual and reproductive health (SRH) services: births assisted by skilled health-care providers, including midwives; births taking place in health facilities; and access to contraception.
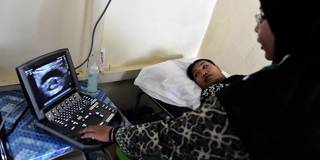
BANGKOK – Last month, Sheuly rushed into a Dhaka hospital in need of emergency treatment. The 25-year-old Bangladeshi woman had just given birth at home – thinking it a safer setting than the hospital during a pandemic. But as she began to suffer from post-partum hemorrhage – one of the leading causes of maternal death worldwide – avoiding exposure to COVID-19 was the furthest thing from her mind. The same was true of Majufa Akter, the midwife who sprang into action and saved Sheuly’s life, despite not having yet received adequate personal protective equipment (PPE).
Giving birth is an intense moment in a woman’s life under any circumstances. Doing so during a pandemic imbues the experience with a new form of stress. Mothers do not know whether to go to hospitals – where they fear exposure to the coronavirus, personnel shortages, or separation from their partners – or to give birth at home, where medical complications often become far riskier. This is just one example of how the imperative of managing the COVID-19 pandemic is complicating the delivery of essential health services – and leaving women, in particular, highly vulnerable.
Around the world, when health systems are overstretched, services for women are often among the first to suffer, resulting in increased maternal and child morbidity and mortality. To illustrate the risks, we have modeled the pandemic’s possible impact on three key sexual and reproductive health (SRH) services: births assisted by skilled health-care providers, including midwives; births taking place in health facilities; and access to contraception.