Much emphasis has been placed on building lab capacity for polymerase chain reaction tests, the gold standard for detecting the COVID-19 virus. But such a strategy is unlikely to prove politically and financially sustainable. And too many people would still die.
CAMBRIDGE – In Massachusetts, which has a population of close to seven million, over 6,000 people have died from COVID-19 since the beginning of March. But one relatively small group – including about 38,000 people, or 0.5% of the state’s population – accounts for 60% of these deaths. This group comprises everyone who lives in nursing homes, and protecting these people and the staff who care for them, all of whom remain highly vulnerable to severe infection, must be a top priority everywhere as economies reopen.
According to pre-pandemic data, the number of people in nursing homes typically averages around 1.3 million across the United States. These older inhabitants are cared for by a workforce that numbers around one million. Fortunately, there is now a better way to reduce significantly their risk of death: implement a focused public-health monitoring program based on all available forms of testing – including the latest serology blood tests for antibodies – for people in and around nursing homes and the broader population.
Much emphasis has been placed on building lab capacity for polymerase chain reaction (PCR) tests, the gold standard for detecting the COVID-19 virus. PCR testing capacity is essential to manage outbreaks. In Massachusetts, heroic technological efforts by the Broad Institute of MIT and Harvard (a biomedical and genomic research organization) helped save many lives by greatly increasing the availability of testing for nursing homes and others early in the pandemic. We need more such leadership throughout the US and around the world.
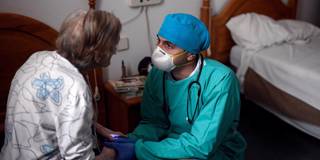
CAMBRIDGE – In Massachusetts, which has a population of close to seven million, over 6,000 people have died from COVID-19 since the beginning of March. But one relatively small group – including about 38,000 people, or 0.5% of the state’s population – accounts for 60% of these deaths. This group comprises everyone who lives in nursing homes, and protecting these people and the staff who care for them, all of whom remain highly vulnerable to severe infection, must be a top priority everywhere as economies reopen.
According to pre-pandemic data, the number of people in nursing homes typically averages around 1.3 million across the United States. These older inhabitants are cared for by a workforce that numbers around one million. Fortunately, there is now a better way to reduce significantly their risk of death: implement a focused public-health monitoring program based on all available forms of testing – including the latest serology blood tests for antibodies – for people in and around nursing homes and the broader population.
Much emphasis has been placed on building lab capacity for polymerase chain reaction (PCR) tests, the gold standard for detecting the COVID-19 virus. PCR testing capacity is essential to manage outbreaks. In Massachusetts, heroic technological efforts by the Broad Institute of MIT and Harvard (a biomedical and genomic research organization) helped save many lives by greatly increasing the availability of testing for nursing homes and others early in the pandemic. We need more such leadership throughout the US and around the world.