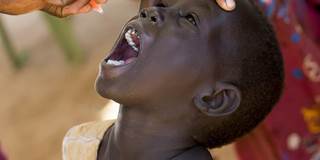
Nigeria has not had a single case of wild polio in the last 12 months. This important achievement provides grounds for optimism, not only in the fight against polio, but for global health efforts in general, showing that it is possible to bring modern medicine to the world’s most marginalized and hard-to-reach children.
GENEVA – It has been a tough year for Nigeria. In the last 12 months, the country has suffered attacks by child suicide bombers and brutal massacres by Boko Haram. The vast majority of the 276 schoolgirls abducted in Chibok last year are still missing. And yet, during this time, despite such horrors, Nigeria has quietly managed to achieve something truly remarkable: an entire year without a single new case of wild polio.
This is a great achievement for Nigeria and all of its partners in the effort to eradicate the disease. Less than 30 years ago, polio plagued 125 countries, paralyzing 1,000 children a day. Until now, there were only three countries where the virus was still considered endemic: Afghanistan, Pakistan, and Nigeria. Health officials wait three years before declaring a country polio-free, but the one-year milestone in Nigeria raises hopes that we may have already seen the last case of wild polio in the country – and the whole of Africa.
In addition to the logistical challenge of reaching every child in Africa’s most populated country, the Nigerian polio-eradication campaign has had to overcome security issues, opposition by religious fundamentalists, and rampant corruption. The fact that a country as troubled as Nigeria could pull off such an important feat is cause for celebration and provides grounds for optimism, not only in the fight against polio, but for global health efforts in general. Nigeria’s success shows that it is possible to bring the miracles of modern medicine to the world’s most marginalized and hard-to-reach children.
GENEVA – It has been a tough year for Nigeria. In the last 12 months, the country has suffered attacks by child suicide bombers and brutal massacres by Boko Haram. The vast majority of the 276 schoolgirls abducted in Chibok last year are still missing. And yet, during this time, despite such horrors, Nigeria has quietly managed to achieve something truly remarkable: an entire year without a single new case of wild polio.
This is a great achievement for Nigeria and all of its partners in the effort to eradicate the disease. Less than 30 years ago, polio plagued 125 countries, paralyzing 1,000 children a day. Until now, there were only three countries where the virus was still considered endemic: Afghanistan, Pakistan, and Nigeria. Health officials wait three years before declaring a country polio-free, but the one-year milestone in Nigeria raises hopes that we may have already seen the last case of wild polio in the country – and the whole of Africa.
In addition to the logistical challenge of reaching every child in Africa’s most populated country, the Nigerian polio-eradication campaign has had to overcome security issues, opposition by religious fundamentalists, and rampant corruption. The fact that a country as troubled as Nigeria could pull off such an important feat is cause for celebration and provides grounds for optimism, not only in the fight against polio, but for global health efforts in general. Nigeria’s success shows that it is possible to bring the miracles of modern medicine to the world’s most marginalized and hard-to-reach children.